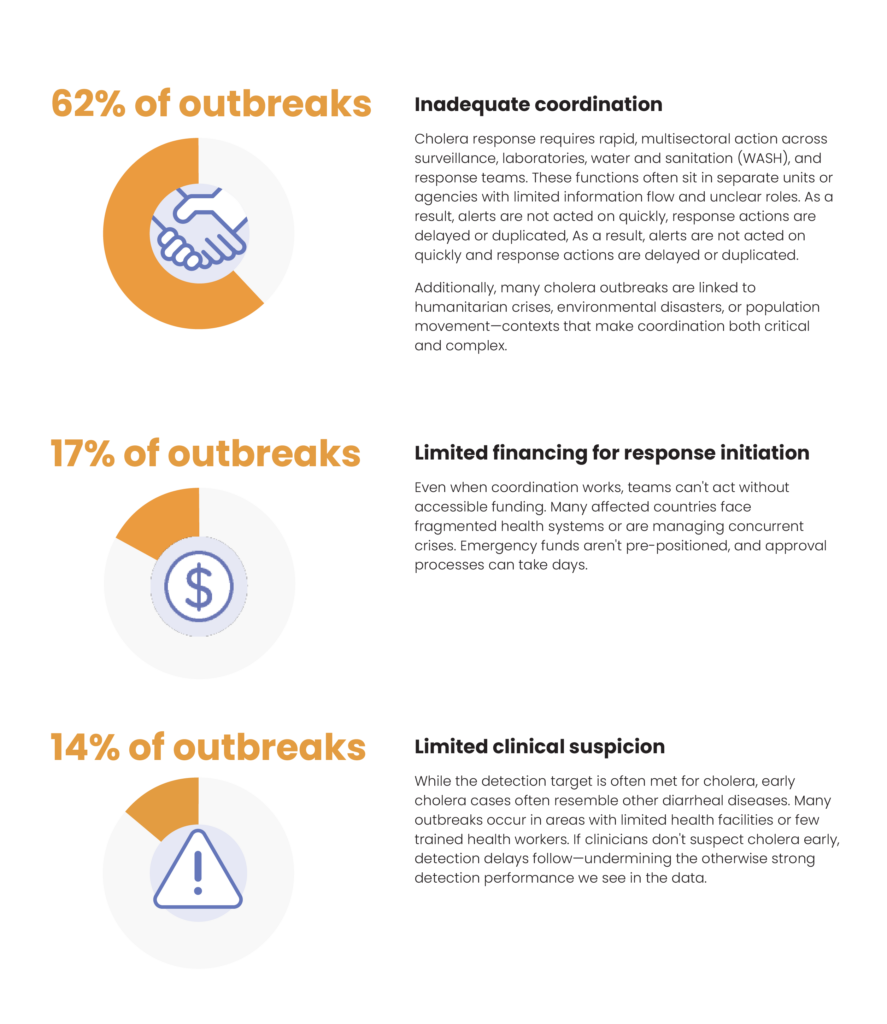
As cholera surges globally, 7-1-7 data from 52 outbreaks across six countries point to a persistent challenge: In nearly two-thirds of cholera responses, coordination constraints delay critical action.
After years of decline, cholera is surging. In 2025, 33 countries reported more than 600,000 cases and 7,500 deaths. The Africa Centres for Disease Control and Prevention have identified cholera as a top challenge, with outbreaks rapidly moving toward a regional health emergency in parts of Africa and the Middle East.
The drivers are clear: humanitarian crises, armed conflict, climate disasters, and populations lacking access to safe water and sanitation. Outbreaks are recurrent, fueled by displacement, health inequities, rapid urbanization, and ongoing conflict. Cholera can kill within hours, but treatment is inexpensive and widely available; after several years of global shortages, supplies of oral cholera vaccines have begun to improve.
7-1-7 data reveals that the main challenge isn’t finding cholera cases; it’s coordinating the multisectoral response needed quickly—and shows countries what to fix.
How cholera performs against the 7-1-7 target
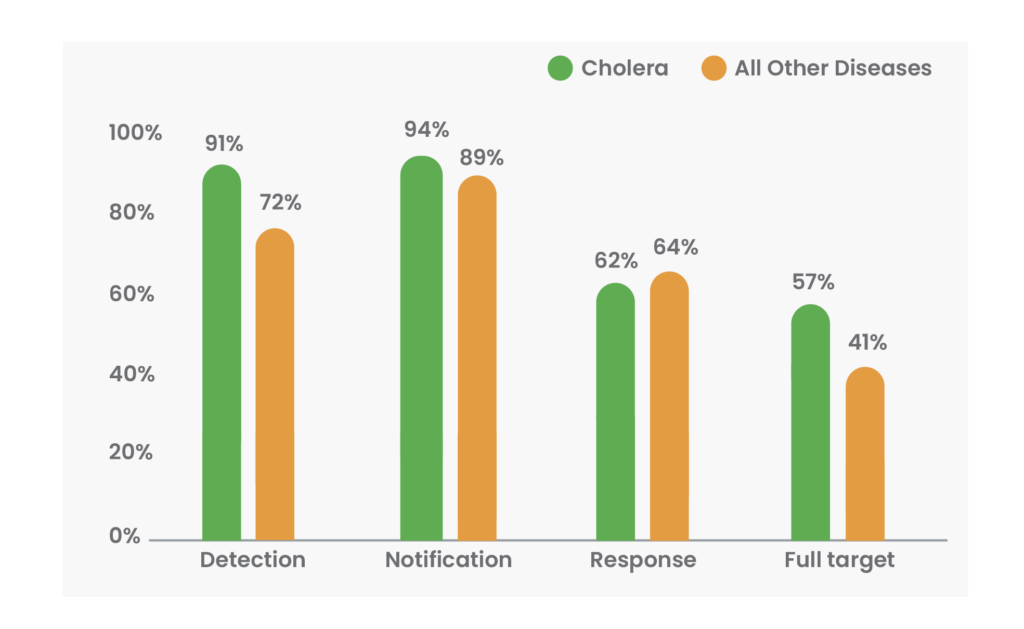
Across the 52 cholera outbreaks from six countries in our analysis, detection and notification performance was strong (90% and 94% of outbreaks met the detection and notification targets, respectively)—among the highest of any outbreak type. But response lagged: only 62% of outbreaks completed early response actions within seven days of notification––a slightly weaker performance than the average across all diseases.
Left: 7-1-7 data shows that one-third of cholera outbreaks missed the early response target
Why response is delayed
Bottlenecks are concentrated in the early response phase, specifically around response initiation and laboratory confirmation. For polio, a disease targeted for global elimination, delays can occur from sample collection to final sequencing to confirm the specific strain (wild-type or vaccine-derived) due to delays in sample collection, transport, and multiple laboratory processing steps following strict criteria.
How we can do better
Achieving the 7-1-7 target for cholera depends on a set of critical enabling factors that support rapid detection, timely reporting, and effective response. These enablers, largely seen in 7-1-7 operational research data from East and West Africa, include strong coordination structures, robust surveillance systems and early detection systems, frontline workforce capacity, reliable access to pre-positioned supplies and financing, and integrated, multisectoral planning. The solutions that follow translate these enabling factors into practical action to drive faster, more coordinated, and more effective cholera responses.
1. Strengthen coordination
Effective multisectoral coordination can’t be improvised during crises. Countries must build structures in advance.
Use 7-1-7 as the shared operational framework to:
- Strengthen subnational emergency operations centers or similar coordination structures for cholera in high-risk regions or hotspots where cholera outbreaks tend to occur.
- Pre-define roles, decision authority, and handoffs across surveillance, labs, WASH, and incident management teams in these regions before outbreaks strike.
- Establish cross-border collaboration protocols, especially along high-mobility corridors where cholera spreads quickly. Conduct emergency response reviews with 7-1-7 data for each outbreak to identify where coordination broke down and adjust actions for immediate performance improvement.
How Thailand contained cross-border cholera
Acting on lessons from past outbreaks means we can stop cholera before it spreads. That’s how Thailand successfully contained a cholera outbreak that began at its border with Myanmar––by implementing recommendations from the 7-1-7 analysis of an earlier E. coli outbreak. Only 10 cross-border cases were identified, and no deaths occurred. Read the full case study in Epidemics That Didn’t Happen.
Embed cholera in national emergency and multi-hazard plans:
- Many countries update national emergency plans annually with multisectoral input. Cholera coordination should be integrated into these plans and the meetings that support them.
- Because cholera outbreaks are often tied to humanitarian or climate disasters, response can become embedded within humanitarian cluster systems. Countries should create and align SOPs for coordination across these systems.
A successful coordinated, multi-sectoral response to cholera in Kenya
When a cholera outbreak emerged in Migori, Kenya, authorities concurrently activated the County Emergency Operations Center, deployed rapid response teams, and released stocks for WASH and medical supplies––allowing them to reach the 7-1-7 target and contain the outbreak to 53 suspected cases, 16 confirmed, and one death. Read the full study.
2. Make emergency funds and supplies immediately accessible
Fully fund national cholera plans and establish contingency financing mechanisms that can be released within a few days for cholera response. Read more on unlocking resources for rapid outbreak investigation.
Pre-position supplies in high-risk and high-mobility areas: vaccines, diagnostics, treatment supplies. When outbreaks hit, response teams shouldn’t wait for procurement processes to start. A recent study has shown that 80% of cholera cases could be averted if cholera vaccination responses start within the 7-1-7 target.
Invest in WASH infrastructure and services as prevention. Safe water and sanitation prevent cholera outbreaks from happening in the first place.
3. Improve clinical suspicion at the frontlines
Strengthen surveillance systems and expand training on cholera case management at health facility and community levels. Don’t wait for outbreaks to train workers.
Embed cholera refresher training into routine supervision for health workers. Standardize simple cholera alert protocols so clinicians know exactly when and how to report suspected cases.
Read more on overcoming low clinical suspicion in outbreak detection.
Nigeria frontline health workers report increased confidence in cholera identification thanks to online training
In June 2024, Nigeria experienced a sudden surge in cholera cases, part of a wider outbreak. By July, the nation reported the highest number of deaths of any country in the region. The Nigerian government and Resolve to Save Lives sprang into action and immediately released an online training module on cholera, allowing health care workers to quickly get up-to-speed on essential signs and symptoms and critical protective measures. Within three days, the training had reached 3,000 health care workers, rising to almost 6,000 within a week. Frontline workers who completed the training saw a 29% increase in their knowledge about cholera, and over 98% reported increased confidence in how to identify and report suspected cases. Read more about the online training developed by Resolve to Save Lives.
A path forward
Efforts of governments, donors and partners are already resulting in timely detection and notification of cholera outbreaks. Data driven strategies to target geographies and improved availability of critical tools like oral cholera vaccines provide an opportunity to further improve response performance. However, consistency is key. Cholera plans should be fully funded, and 7-1-7 should be embedded into emergency systems––to identify and fix bottlenecks in near real time. Lastly, countries should strengthen and track their investments in WASH and surveillance.
Join the 7-1-7 Global Community of Practice
This is where countries share real experiences, and collective problem-solving accelerates progress on outbreak response performance.